Public Health
The WHO Red List Nigeria Status: A Healthcare System Analysis
The WHO’s red list for Nigeria is more than a label. It’s the story of morning queues at hospitals, empty drug shelves, and a system straining under its own weight. This is a look at the daily…
The WHO Red List Nigeria Status: A Healthcare System Analysis
Published: 11 March, 2026
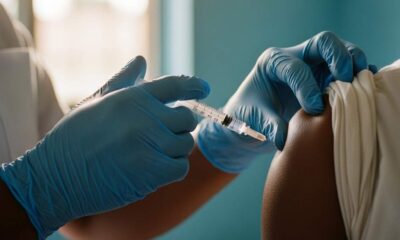
March 2024 was when the World Health Organization last updated its list, the one many people just call the red list. It is a dynamic tool, they say, meant to protect fragile health systems from having their professionals actively recruited away to other countries. The intention is a shield, a form of international courtesy that acknowledges a critical shortage. But standing in the queue outside a tertiary hospital gate, which forms faithfully before seven in the morning, you see a different kind of protection. It is the quiet, daily endurance of people waiting for care in a system that has been straining at the seams for a very long time.
This red list status is not an abstract label from Geneva. It identifies countries where the density of doctors, nurses, and midwives falls below the global median, where the index for universal health coverage service misses its mark. The catch, the small print that everyone knows, is that while the status aims to shield Nigeria from poaching, it primarily reflects deep, homegrown gaps in the very foundation. These are the gaps that quietly fuel the brain drain, creating a vacuum that the list itself cannot fill. The professionals leave not just because someone asks them to, but because the conditions here often ask them to leave.
The Measurable Gaps
Let us talk about what you can count, because the numbers have a cold, clear voice. In the 2026 federal budget, the allocation for health sits at 4.6% of a total ₦49.74 trillion. That figure is a long way from the 15% target pledged in the Abuja Declaration, a promise that now feels like a conversation from another era. This financial shortfall is the bedrock of every other problem. It cripples what officials call commodity security, which is just a technical term for having the right drugs on the shelf when you need them. The result is a crushing burden shifted onto families, where out-of-pocket expenditures account for a significant majority of all health spending. You pay, often through the nose, for what the system cannot provide.
The technical capacity to detect disease often lags, too. An assessment by the Federal Ministry of Health notes that laboratory diagnostic speed for zoonotic diseases continues to be below benchmark. Surveillance systems are improving but still struggle with full digital integration, with persistent manual reporting in some areas causing delays. In remote local government areas, handwritten notes in file jackets can delay the consolidation of vital national statistics for weeks. This is not just about paperwork. It is about a chain of information that breaks, and when it breaks, disease detection slows down. Time, in matters of health, is a currency we are always short of.
The Empty Shelf
Walk into many primary healthcare centres and the reality is stark, almost physical. Data from the National Bureau of Statistics reveals that only a fraction of sampled health facilities have essential, unexpired drugs available. Supply chain failures are not an exception. They are routine. Then consider that only about 48% of healthcare facilities in Nigeria have access to basic water services. Now think about treating cholera, or any infection, without clean water. The shelf is empty, the tap is dry, and the nurse is overwhelmed.
The human resource base is fractured. A study from the WHO African region shows Nigeria operates with a dangerously low density of healthcare workers per one thousand population, which is less than half of what the WHO recommends for basic universal health coverage. The deficit is most acute in rural areas, where a single nurse might serve thousands of people across scattered villages. They become islands of care in a vast sea of need, and the pressure is enough to make anyone consider a life elsewhere. This is the arithmetic of the red list, written not in reports but in the tired eyes of the people who stay.
Contrast this with the pockets of progress, because they do exist and they matter. The Nigeria Centre for Disease Control and Prevention has successfully deployed a digital surveillance and outbreak response management system across all states. The laboratory network has expanded, with the National Reference Laboratory in Abuja becoming a center for genomics. These are real advances, fragile threads of hope in a frayed fabric. Yet they depend on a steady supply of reagents and consistent electricity, two things that are often in short supply. The most sophisticated machine in the world is just a paperweight when the power goes out.
The Relentless Outbreaks
The epidemiological data does not lie, and it tells a story of relentless pressure. In 2025, Nigeria recorded 93,453 suspected cholera cases with 3,161 deaths. For Lassa fever, the count was 906 confirmed cases with 168 deaths as of a specific week in 2025. These are not just statistics. They are families, communities, and health workers pushed to the limit. The red list aims to streamline the international response to such outbreaks, to marshal global help more efficiently. But the unspoken goal, the quiet hope, is to build local capacity so we are not perpetually waiting for external saviors. The aim is to shorten the queue outside the gate with our own hands.
“The strength of a health system lies in its ability to generate and use information at the point of collection. Our focus continues to be making data work for the people at the front lines.”
– Dr. Muyi Aina, Executive Director of the National Primary Health Care Development Agency.
The path forward, as the good doctor implies, is granular, not grand. It involves formalizing simple data review meetings at the local government level. Imagine a core unit—the local health department head, surveillance officers, primary healthcare coordinators—sitting monthly in a basic facility. They review reports. They turn raw numbers into local intelligence, generating a concise summary for state ministries that highlights specific bottlenecks like drug stock-outs or broken refrigerators. This is the unglamorous work of repair. It is about making the system see itself clearly, one detail at a time.
The WHO red list status for Nigeria is a reflection in a mirror we sometimes wish was kinder. It is also a guide, a map of the canyons we need to bridge. By addressing these technical areas incrementally, fixing the data flow, ensuring the drugs are on the shelf, making the workplace one professionals want to stay in, the system builds resilience. Each small improvement is a brick in a longer, stronger bridge between a diagnosis and an action. The work is in the details, and in a place where so much is broken, the details are everything. They are the difference between a queue that grows and one that, slowly, begins to shrink.


Public Health
Local Herbal Drink Side Effects and Popular Brands in Nigeria
You see them in traffic and markets. Brightly colored bottles promise relief from pile or malaria. These local herbal drinks form a multi-billion naira industry, but what’s really in them?


Local Herbal Drink Side Effects and Popular Brands in Nigeria
Published: 03 April, 2026
You see them in traffic, in markets, and in corner shops. Brightly colored bottles with labels promising relief from pile, stomach pain, or malaria. These local herbal drink concoctions, often called Agbo, form a multi-billion naira informal industry. A 2025 report in Premium Times noted that the National Agency for Food and Drug Administration and Control has registered over 13,000 herbal medicines. The actual number of unregistered products circulating in the market remains a mystery.
Here is the thing. Many consumers believe these products are inherently safe because they are natural. This belief drives a massive, mostly unregulated market. A report from the World Health Organization in 2025 noted that up to 80% of the population in some African countries uses traditional medicine for primary healthcare. In the context of Nigeria, this translates to a heavy reliance on these bottled mixtures.
What Is Actually In The Drink
Let us break it down. A typical local herbal drink contains a blend of roots, barks, leaves, and seeds. Common ingredients include ginger, garlic, lemon grass, and bitter kola. The problem starts with preparation because there is no standard dose. One maker uses a handful of leaves while another uses two.
Scientific analysis reveals more. A 2025 study published in the Journal of Ethnopharmacology tested 45 popular Agbo samples from Lagos markets. The study reported that 34% of the samples contained undeclared pharmaceutical drugs, including painkillers and steroids. Another 23% had heavy metal contamination above safe limits. You are drinking more than herbs.
Brands You Know And The Risks They Carry


So here we are. You recognize the names. Brands like Agbo Jedi Jedi for pile, Opa Eyin for eye issues, and Agbo Ibà for fever dominate the landscape. These products have become household names through word-of-mouth and aggressive street marketing. Their efficacy is an article of faith for many.
Yet, clinical evidence is scarce. The side effects range from mild to severe. Common complaints include acute stomach upset, diarrhea, and dizziness. More serious cases involve liver damage and kidney injury. A 2026 report in The Guardian Nigeria noted that a teaching hospital in Ibadan documented a 15% rise in cases of liver toxicity linked to herbal medicine from 2024 to 2025. The patients cited popular brand names.
The Liver And Kidney Question
The liver processes everything you consume. Some herbs contain compounds that are toxic to liver cells with prolonged use. The kidney filters waste from the blood. Contaminants like heavy metals accumulate and cause irreversible damage. These organs work silently, so damage often goes unnoticed until it becomes critical.
Professor Abdulsalami Nasidi, a public health consultant, highlighted this point.
“The absence of immediate adverse effects creates a false sense of security. Chronic toxicity from repeated consumption of unstandardized herbal mixtures presents a silent public health challenge.”
– Professor Abdulsalami Nasidi, public health consultant, in The Nation (March 2026)
The Regulatory Gap Is A Canyon
NAFDAC has a mandate to regulate all consumables. The agency operates a registration process for herbal medicines. Manufacturers submit details about their ingredients and production process. Upon approval, they receive a registration number for their label.
Reality check. The informal market is vast. Many producers operate without any registration. Even for registered products, post-market surveillance is weak. In 2026, NAFDAC has intensified its “Yellow Label” initiative for verified traditional medicines. This specific identifier helps consumers distinguish certified products from unregulated ones. However, a 2025 report in BusinessDay noted that a NAFDAC director conceded at a stakeholders meeting that logistical challenges continue to hinder comprehensive market monitoring. The system relies heavily on complaints before investigation.
Why Enforcement Stumbles
Think about the supply chain. Production happens in small, scattered workshops. Distribution uses thousands of informal vendors. This decentralized model makes tracking difficult. Enforcement officers focus more on large-scale, packaged food and drug fraud. The woman selling single bottles in a basket often escapes scrutiny.
Cultural acceptance also shields the industry. Many citizens view regulation as government interference in traditional practice. This sentiment creates a social barrier for effective control. The seller is a neighbor providing a trusted service, not a criminal.
Stories From The Hospital Ward


Medical doctors have stories. Dr. Chioma Mbonu, a gastroenterologist in Abuja, sees the consequences. She recounted a case from late 2025. A man in his forties came with severe jaundice and abdominal pain. He had consumed a popular local herbal drink for stomach ulcers for three months. Tests confirmed drug-induced hepatitis linked to the herbal mixture.
“Patients often do not disclose herbal use during consultation. They consider it irrelevant or fear judgment. This information gap delays correct diagnosis and appropriate treatment.”
– Dr. Chioma Mbonu, gastroenterologist, interview with Vanguard (February 2026)
These cases are underreported. Patients seek care at traditional healers first or use another herbal mix to counter the side effects of the first. By the time they reach a conventional hospital, the condition is advanced.
The Economic Pull Is Strong
Forget the health talk for a minute. This is about livelihood. Selling Agbo provides income for countless families. The barriers to entry are low. You need some knowledge of herbs, bottles, and a small capital. This economic reality guarantees the market continues to thrive.
The appeal is also financial for the consumer. A bottle of Agbo costs a fraction of a doctor consultation fee or prescribed antibiotics. In an economy with high out-of-pocket health expenditure, this price difference is decisive. People manage their health with the resources they have.
A Path Forward Exists
This situation requires a pragmatic solution. A wholesale ban would fail and push the trade further underground. The goal should be harm reduction and quality improvement. Integration of traditional medicine into the formal health system offers a viable model.
NAFDAC launched the Herbal Medicine Product Registration Acceleration Initiative in 2024. The program aims to bring more producers into the regulatory fold by simplifying paperwork. According to the NAFDAC Official Bulletin in 2026, the agency reported a 20% increase in applications from herbal practitioners as of March of that year. This is a positive step, but scale is necessary.
What You Can Do Today
Your health is your responsibility. You make choices every day. If you choose to use a local herbal drink, apply basic consumer wisdom.
- Look for the NAFDAC registration number on the label. A missing number is a red flag.
- Look for the “Yellow Label” — NAFDAC’s 2026 initiative for verified traditional medicines.
- Purchase from reputable vendors, not random hawkers.
- Listen to your body. Discontinue use if you experience unusual symptoms like prolonged nausea, yellow eyes, or reduced urination.
- Inform your doctor about every substance you ingest, including herbs. This disclosure helps them protect you.
The Final Word On Herbal Drinks
Traditional medicine has a place in the culture of Nigeria. It offers accessibility and cultural resonance. The challenge lies in ensuring its safety for the population. The current system, with its gaps, exposes millions to preventable risk.
Progress depends on collaboration. Regulators, practitioners, and consumers each have a role. Producers must embrace standardization. Authorities must enhance monitoring. Citizens must demand quality. The story of local herbal drink in Nigeria is still being written. The next chapter needs more science and less guesswork.
Public Health
Nigeria Hypertension Risk: Urban Diets and Exercise Extend Lives
Hypertension was a major killer in Nigeria’s cities. New 2026 data shows a quiet shift, as urban diets change and sidewalks fill with walkers. These simple choices are starting to bend a deadly curve…


Nigeria Hypertension Risk: Urban Diets and Exercise Extend Lives
Published: 25 March, 2026
Thirty-five per cent of adults in Nigeria had high blood pressure last year, a number that sits in the room like a heavy, uninvited guest. It was the major killer, a quiet crisis built over decades of urban life with its greasy fast food and desk-bound roles. First-quarter data for 2026, however, suggests a subtle shift is happening in the cities, where deliberate changes in kitchens and on sidewalks are starting to bend that deadly curve and add years to urban lives.
The Quiet Kitchen Revolution
So what changed? Look first to the kitchen, where a pragmatic revolution is less about formal diets and more about simple substitution. Health concerns and the rising cost of living are the main drivers, pushing a general trend of Nigerians reducing their consumption of processed foods. People are quietly returning to swallows like amala and eba, but with more vegetable soups and less oily stews, according to Dr. Chioma Nwakanma, a public health nutritionist in Lagos. The awareness is finally sinking in, one pot at a time.
“The data from our community screenings in Surulere and Ikeja shows a 15% lower prevalence of stage 2 hypertension among adults who report high vegetable consumption, compared to those who do not. The message about reducing palm oil and salt is getting through, one kitchen at a time.”
– Dr. Chioma Nwakanma, interview with The Guardian, February 2026.
Supermarket aisles tell the same story, with sales of low-sodium stock cubes and salt substitutes seeing a significant increase. This change is often driven by urbanites who have received a hypertension diagnosis, a reaction that slowly hardens into a new habit.
Walking the Talk
Now look outside, where exercise is ceasing to be a foreign concept entirely. The most significant change is the simple normalization of walking. In Abuja, Millennium Park and the green areas in Maitama are filled with walkers at dawn, while in Lagos, the state government’s cleanup of sidewalks in Ikoyi and Victoria Island has made the simple act less of a hazardous adventure. Organized running clubs have exploded in popularity, from the flagship Access Bank Lagos City Marathon to weekly park runs in Port Harcourt, turning physical activity into a social event that corporate wellness programs are now eagerly promoting.
A Fragile Progress
Preliminary data is starting to show results, with an interim report by the Nigeria Centre for Disease Control pointing to a stabilization in hypertension rates among urban adults under 50. Contrast this with World Bank data from 2023 that put average life expectancy at about 54.5 years, and you begin to see the tangible impact of these lifestyle modifications in preventing cardiovascular events.
“Our models suggest the lifestyle modifications in cities, less dietary salt, more aerobic activity, are directly preventing cardiovascular events. For every 10% increase in reported moderate exercise in a population, we see a correlating 2-3% drop in hypertension-related hospital admissions. The link is evident.”
– Prof. Ibrahim Danjuma, African Journal of Medicine, December 2025.
There is a catch, of course. This progress is fragile and concentrated among the educated, middle-class urban population. The urban poor, in crowded estates with limited access to fresh food and safe spaces, continue to be extremely vulnerable, their risk unchanged or even worsening while government policy moves at a glacial pace.
The Policy Gap
One simple policy could change the game: mandatory hypertension screening at every primary health contact. Go to a clinic for malaria, get your blood pressure checked. The reality, however, is more complex. While 98% of urban Primary Healthcare Centers have working blood pressure apparatus, only 24% have the clinical guidelines to treat the patients they diagnose. This readiness gap is the missing link, even though a pilot program in Lagos showed a 300% increase in new case detection and linked 65% of those diagnosed to care.
The most practical step for you is personal and immediate. A blood pressure check takes two minutes and is often free at pharmacy outlets in major cities. Make that check this week, because if the reading is high, that information becomes power. It starts a conversation that can motivate one less stock cube in the pot or justify a 30-minute walk. The entire national change, after all, is built on millions of small decisions just like that one.
Public Health
Lassa Fever in Nigeria: The 2026 Numbers and Realities
The NCDC’s 2026 report shows 506 Lassa fever cases and 95 deaths in eight weeks, with a 24.5% fatality rate. Five states bear 84% of the burden in a familiar, grim cycle tied to ecology and living…


Lassa Fever in Nigeria: The 2026 Numbers and Realities
Published: 23 March, 2026
Five hundred and six cases. That was the official count from the Nigeria Centre for Disease Control and Prevention for just the first eight weeks of 2026, a number that carries the weight of ninety-five deaths before the year had properly settled in. The trajectory feels grimly familiar, like an old story you hear every dry season when the rodent Mastomys natalensis becomes more active around human homes. What makes you pause this time is the Case Fatality Rate of 24.5% for confirmed cases, a figure the NCDC itself noted was higher than the historical average in its weekly report.
The Usual Suspects
Five states bear the overwhelming burden, a pattern so entrenched it feels like a permanent feature on the map. Bauchi, Ondo, Taraba, Edo, and Benue account for 84% of all confirmed infections, with Bauchi alone responsible for 30% of the cases. Eighteen states in total have recorded at least one case, showing how widely the virus has spread its roots, primarily through contact with infected rodent excreta in food stores. You look at the breakdown and see not just statistics but a geography of recurring distress.
Counting the Fever
The system for tracking this has its own rhythm. A suspected case triggers an investigation, samples travel to National Reference Laboratories, and a positive PCR test confirms Lassa fever. Data flows from treatment centers to state teams and finally to the national agency, where weekly reports paint the picture. Dr. Jide Idris, the Director-General of the NCDC, framed the ongoing mission in a briefing covered by The Guardian.
“Our focus remains on early detection, effective case management, and risk communication. The collaboration with state ministries of health is critical for interrupting transmission.”
– Dr. Jide Idris, NCDC Director-General, February 2026.
The Treatment Puzzle
The cornerstone of treatment is the antiviral drug Ribavirin, and timing is everything because patients who get it within the first six days of symptoms have a far better chance. Access, however, remains a persistent logistical puzzle that the NCDC stockpile for designated treatment centers tries to solve, though a 2025 study highlighted critical gaps with some centers reporting stock-outs. Specialized isolation wards and protective gear are not just items on a list but the thin line between containment and spread.
Why It Comes Back
The ecology writes the script. The dry season from December to April sees increased rodent activity in human dwellings, aided by harvested crops like maize left near homes and construction materials like mud walls that offer easy entry. Cultural practices persist, with many households keeping grain in sacks inside living areas, and the perception battle adds another layer. As Premium Times reported, some residents view the fever as a spiritual affliction long before considering a biomedical cause, a conflict fought anew every season.
The Cost of Containment
This brings us to money, always a revealing part of the story. The 2026 appropriation act earmarked N2.46 trillion for the entire health sector, about 4.23% of the total national budget, but the specific allocation for Lassa fever response remains opaque within broader line items. Funding flows through the NCDC and state budgets with support from international partners, yet the gap between appropriation and reality is stark. Health Minister Mohammed Pate revealed that only ₦36 billion was received out of the ₦218 billion appropriated for 2025, a discrepancy that prompted a new policy for 2026 to try and prevent delays.
Behind the Numbers
Behind the 95 fatalities are families and front-line workers, each death signaling a breakdown in a system under strain. Healthcare workers are directly in the line of fire, with confirmed infections among them remaining a challenge in 2026, often happening in hospitals without proper isolation or gear. A medical director in Ondo State, speaking anonymously, put a face on the loss.
“We lost a senior nurse in our facility. She was the backbone of our maternity ward. The outbreak empties our wards of other patients and drains the morale of the staff.”
– Anonymous medical director, Ondo State, March 2026.
The economic devastation for affected households, from treatment costs to lost income, completes a picture of layered hardship.
Beyond the Annual Cycle
Sustainable control requires moving beyond reaction to investment in environmental sanitation and rodent-proofing homes, while research into a vaccine continues slowly. Community engagement needs a new model, and the structure of the health system itself complicates everything because primary healthcare centers often cannot diagnose Lassa fever. Patients travel long distances to tertiary centers, a delay that reduces Ribavirin’s efficacy and increases risk, creating a cycle that feels difficult to break.
What You Can Do
Store food grains in metal containers with tight lids, seal holes and cracks in your walls, and dispose of garbage in covered bins to maintain a clean environment. Seek medical attention immediately for a persistent fever with headache and weakness because early presentation saves lives, and avoid contact with blood and body fluids of a sick person while using gloves if providing care before reaching a hospital. These simple actions form a personal front line in a larger battle.
The NCDC reports provide a vital, grim snapshot of persistence, a disease entrenched in ecology and living conditions that demands a fundamental shift. The dry season will end, the rains will come, and the case counts will fall until the dashboard shows green, waiting quietly for the cycle to begin again next December.



 Digital Sovereignty2 months ago
Digital Sovereignty2 months agoInternet Sovereignty: Why Some Countries Want Their Own Separate Internet



 Technology & Innovation2 months ago
Technology & Innovation2 months agoThe Story Of The Nigerian Who Helped Build Global Internet Systems



 Crime2 months ago
Crime2 months agoNigerian Hackers: The Global Fraud Story and Its Fallout



 Space Technology2 months ago
Space Technology2 months agoForgotten Satellites Defy Silence, Beaming Signals for Decades



 Business2 months ago
Business2 months agoYour Digital Store in Nigeria and the Reality of Domain Expiration



 Maritime2 months ago
Maritime2 months agoThe Phone Stay So Quiet: An Investigation into Nigeria’s Silent Customer Lines



 Business2 months ago
Business2 months agoThe Business That Died: A Nigerian Case Study in Refusal to Adapt



 Business2 months ago
Business2 months agoHiding Your Business From People With Money