Healthcare Crisis
Medical Emergency in Nigeria: Surviving Through Luck or Divine Intervention
Here is the thing. A medical emergency hits. The system groans. You wait. Equipment fails. So here we are. Survival becomes a question of chance. Or something more.
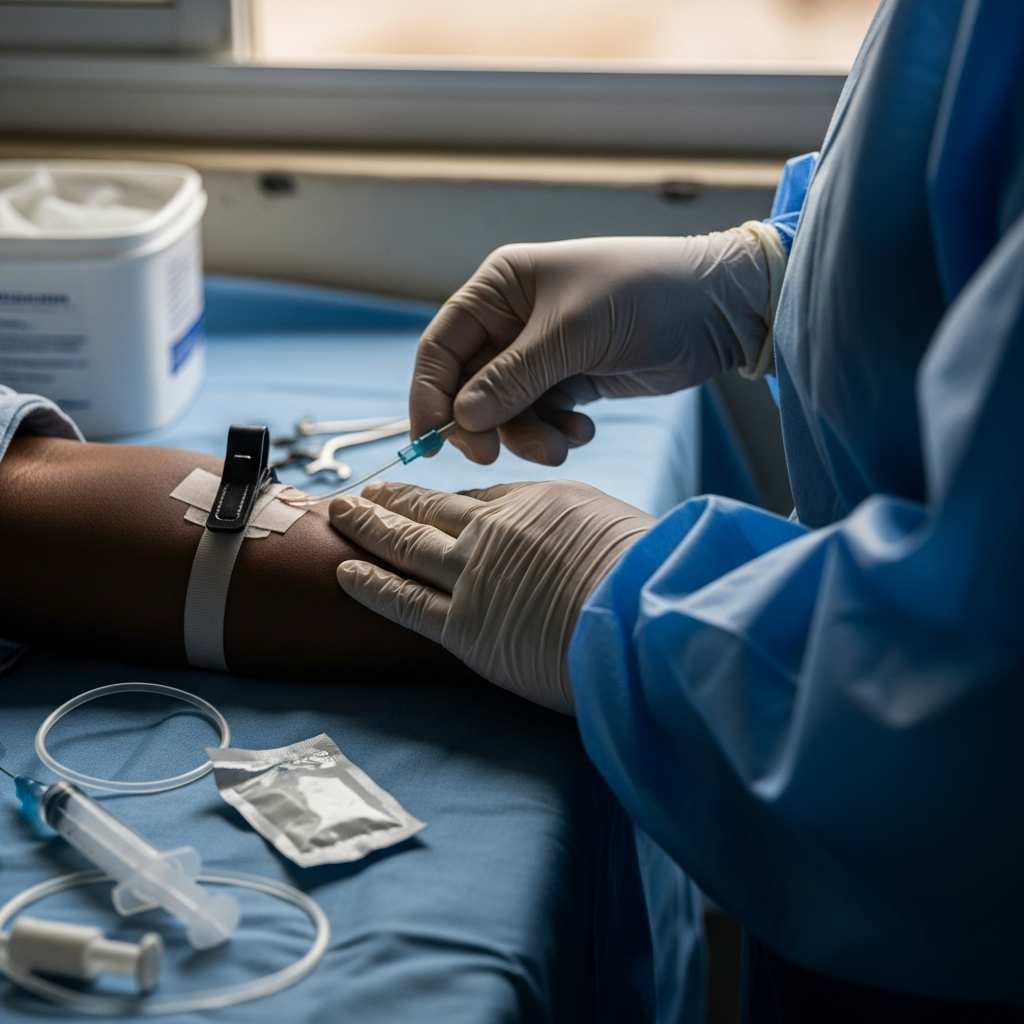
Medical Emergency in Nigeria: Surviving Through Luck or Divine Intervention
Published: 21 March, 2026
What happens in the first sixty minutes after a heart attack on the outskirts of Kano or a car crash in rural Bayelsa? The answer has little to do with medicine. It hinges on a brutal calculus of cash, location, and random chance. The system functions not as a responder but as a filter.
The First Sixty Minutes Are a Lottery
The golden hour is a myth in most places. A functional ambulance service is an urban legend. The Federal Ministry of Health reported in 2023 that fewer than 5,000 operational ambulances serve a population exceeding 220 million people. As Premium Times noted that year, that is roughly one ambulance for every 44,000 citizens.
The distribution skews toward cities. Vast rural areas have zero coverage. People rely on commercial motorcycles, private cars, and sheer goodwill.
But there is a catch. Even if a vehicle is found, there is a second crisis. Poor roads, traffic gridlock, and no emergency lanes turn short distances into marathons. A 10-kilometer trip can take over 90 minutes in Lagos or Abuja during peak hours. The Guardian documented this in February 2026.
What Waits at the Hospital Gate
Arrival offers little reprieve. Your first official interaction is with a finance officer, not a triage nurse. The policy is “cash before care.” It is an unyielding gatekeeper.
A 2024 survey by BusinessDay found that 78% of public hospitals require a deposit before starting emergency treatment. The sums are impossible. For a suspected appendicitis, it is N50,000 to N150,000. For a major accident, hospitals demand upwards of N500,000 as a guarantee. Families make frantic calls and beg at the gate while a patient bleeds.
“We have guidelines, but the reality is that hospitals cannot absorb the cost of unpaid bills. The system collapses if we treat everyone without assurance of payment.” A senior administrator at a federal teaching hospital, speaking anonymously in March 2026.
The time spent negotiating consumes the remaining window for intervention.


The Hollow Core of Health Insurance
The National Health Insurance Authority (NHIA) is the official alternative. Its coverage tells a different story. As of the latest 2023 data, the NHIA covers approximately 16 million Nigerians. That is about 7% of the population.
The vast majority, including the informal sector, have no safety net. Wait, it gets more complex. For the few with insurance, emergencies are fraught with limits. Many plans impose co-payments. They have exclusion lists and caps. A comprehensive plan is N500,000 annual limit can be exhausted by one night in intensive care.
Doctors Without Tools
Assume a patient surmounts the financial hurdle. They then face a depleted system. The doctor-to-patient ratio is estimated at 1 doctor to over 5,000 patients. The World Health Organization recommends 1:600.
The shortage is compounded by a continuous brain drain. The Nigerian Medical Association stated that over 4,000 doctors left the country in 2023 alone, as Vanguard reported in 2024. Emergency rooms are staffed by exhausted professionals.
Basic diagnostics are a luxury. A 2022 assessment of secondary healthcare facilities across 20 states found that 65% lacked functional CT scanners. 80% had broken or obsolete ultrasound machines. Doctors make life-altering decisions based on intuition, not confirmed imaging.
The Budget Tells Its Own Story
The foundation of this crisis is budgetary. Based on the 2026 budget, the allocation to health is N1.33 trillion. The total budget is N49.74 trillion. It falls persistently below the 15% commitment made in the 2001 Abuja Declaration.
Per capita, the federal health budget translates to roughly N6,000 per Nigerian per year. Much is consumed by salaries. Little is left for infrastructure and emergency systems. In 2025, only about 65% of the capital health budget was disbursed for equipment. The funds often never arrive.
Funding for primary healthcare centers, the first line of defense, is particularly anemic. They lack ambulances, personnel, and drugs to stabilize emergencies.
“We have a pyramid that is inverted. We spend on tertiary care in cities, but the base of the pyramid, the primary centers that should prevent emergencies, is crumbling.” Dr. Muyi Aina, Executive Director of the National Primary Health Care Development Agency, in February 2026.
A Map of Survival Odds
Geography dictates destiny. Survival rates vary wildly between states. The National Bureau of Statistics indicated in 2025 that trauma mortality within 24 hours of hospital admission was three times higher in the North-East compared to the South-West.
This links directly to the concentration of specialist centers, paved roads, and networks. An accident on a remote road in Zamfara presents different odds than the same accident on the Lagos-Ibadan expressway.
The urban-rural divide is a chasm. In cities, private hospitals offer an escape route for those with means. They have modern equipment and specialists. Their fees place them beyond most citizens. They exist as a parallel system.

The Social Fabric as a Net
In the absence of a state safety net, Nigerians rely on social and religious networks. The first response is often a broadcast on WhatsApp groups, church assemblies, or mosque congregations. These networks raise funds, provide transport, offer moral support.
This community action is both resilience and an indictment of systemic failure. It transforms healthcare from a right into a charity. The speed and size of one’s social capital become critical.
Faith plays a visible role. Prayers are offered at accident scenes. This reliance on divine intervention is a logical response to a system that has proven unreliable. When science and the state are absent, people look heavenward.
One Practical Shift
A single, actionable change involves the protocol at public hospital gates. The federal and state ministries of health can mandate a “stabilize first, bill later” policy for genuine emergencies. This is enshrined in the National Health Act of 2014, which technically criminalizes refusal of emergency treatment.
Implementation demands a backup financing mechanism, like an emergency care fund. It could be seeded from a tiny percentage of the health budget. This shifts the priority from accounting to medicine in the first critical hour.
This change would not fix the ambulance shortage or the CT scanner. It would remove the most immediate and cruel barrier between a dying patient and a doctor. It replaces the finance officer with a medic at the point of entry.
The Arithmetic of Luck
Surviving a medical emergency here is a complex equation. Variables include proximity to a functional facility, liquidity of funds, competence of staff, functionality of equipment. The constant is chance.
The system, as structured, is a filter that sorts citizens by wealth and location. Those who survive often do so because a random set of circumstances aligned. A relative was nearby with cash. A doctor who trained abroad was on duty. A critical machine was working that day.
This reliance on serendipity is the opposite of a healthcare system. A system implies predictability and guaranteed access. What exists is a patchwork of contingencies.
The conversation about divine intervention arises because the human systems have left a vacuum. When the state is absent in the critical hour, people fill the void with faith, community, and hope against the arithmetic of probability.
The data shows a trajectory of stagnation. The budget percentages low. The doctor exodus continues. Infrastructure decays. Each emergency becomes a fresh test of individual fortune, a stark reminder that in the most vulnerable moment, one’s life depends on a roll of dice.
Rising Star’s Death Sparks Outrage: Can Nigerians Survive Medical Emergencies? , Nigerian Tribune. (Digital Illustration: GoBeyondLocal)





 Digital Sovereignty2 months ago
Digital Sovereignty2 months agoInternet Sovereignty: Why Some Countries Want Their Own Separate Internet



 Diaspora2 months ago
Diaspora2 months agoThe Story Of The Nigerian Who Helped Build Global Internet Systems



 Crime2 months ago
Crime2 months agoNigerian Hackers: The Global Fraud Story and Its Fallout



 Space Technology2 months ago
Space Technology2 months agoForgotten Satellites Defy Silence, Beaming Signals for Decades



 E-Commerce2 months ago
E-Commerce2 months agoYour Digital Store in Nigeria and the Reality of Domain Expiration



 Edutech Portal2 months ago
Edutech Portal2 months agoThe Phone Stay So Quiet: An Investigation into Nigeria’s Silent Customer Lines



 Edutech Portal2 months ago
Edutech Portal2 months agoThe Business That Died: A Nigerian Case Study in Refusal to Adapt



 Business2 months ago
Business2 months agoHiding Your Business From People With Money


























