HealthCare
Medical Emergency in Nigeria: Surviving Through Luck or Divine Intervention
Can you survive a medical emergency in Nigeria? The 2026 data reveals a fractured system where life often depends on luck or divine intervention.
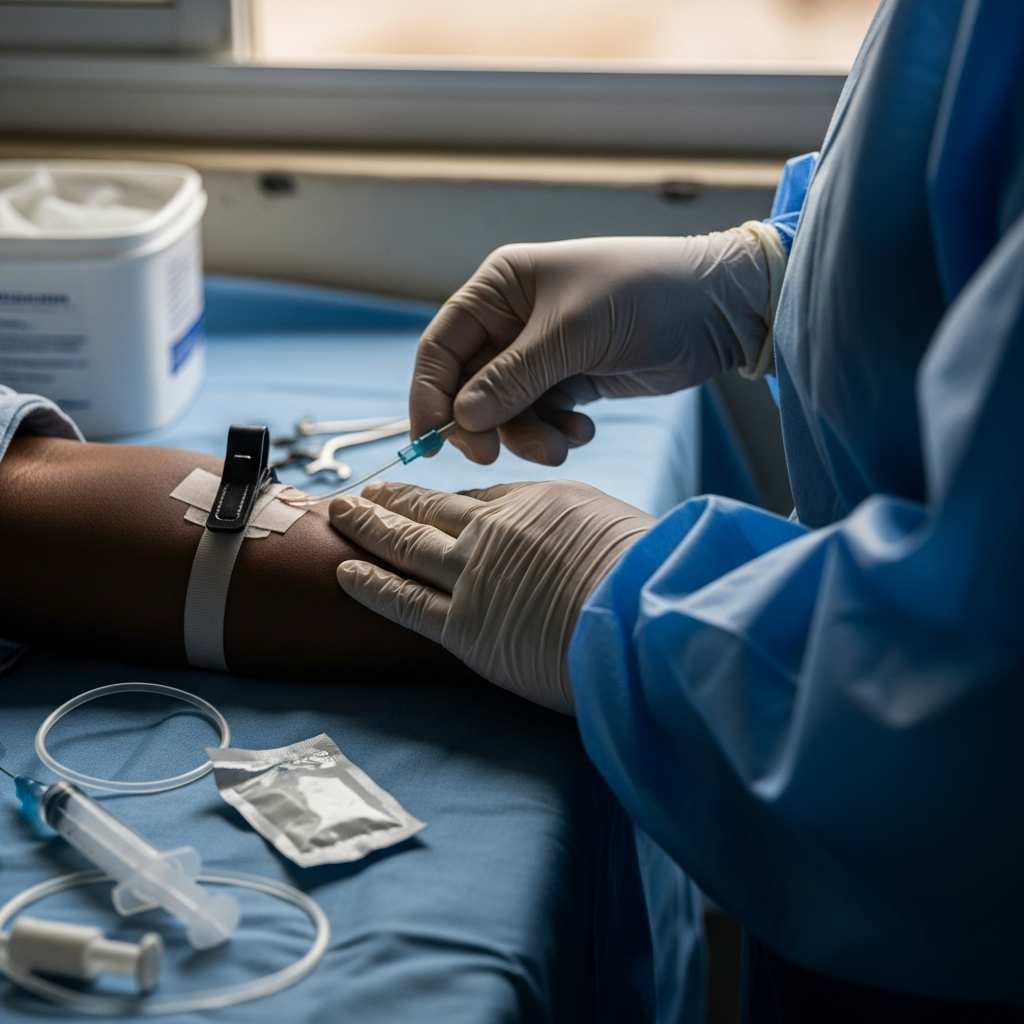
Medical Emergency in Nigeria: Surviving Through Luck or Divine Intervention
Published: 21 March, 2026
What happens in the first sixty minutes after a heart attack on the outskirts of Kano or a car crash in rural Bayelsa? The answer has little to do with medicine. It hinges on a brutal calculus of cash, location, and random chance. The system functions not as a responder but as a filter.
The First Sixty Minutes Are a Lottery
The golden hour is a myth in most places. A functional ambulance service is an urban legend. The Federal Ministry of Health reported in 2023 that fewer than 5,000 operational ambulances serve a population exceeding 220 million people. As Premium Times noted that year, that is roughly one ambulance for every 44,000 citizens.
The distribution skews toward cities. Vast rural areas have zero coverage. People rely on commercial motorcycles, private cars, and sheer goodwill.
But there is a catch. Even if a vehicle is found, there is a second crisis. Poor roads, traffic gridlock, and no emergency lanes turn short distances into marathons. A 10-kilometer trip can take over 90 minutes in Lagos or Abuja during peak hours. The Guardian documented this in February 2026.
What Waits at the Hospital Gate
Arrival offers little reprieve. Your first official interaction is with a finance officer, not a triage nurse. The policy is “cash before care.” It is an unyielding gatekeeper.
A 2024 survey by BusinessDay found that 78% of public hospitals require a deposit before starting emergency treatment. The sums are impossible. For a suspected appendicitis, it is N50,000 to N150,000. For a major accident, hospitals demand upwards of N500,000 as a guarantee. Families make frantic calls and beg at the gate while a patient bleeds.
“We have guidelines, but the reality is that hospitals cannot absorb the cost of unpaid bills. The system collapses if we treat everyone without assurance of payment.” A senior administrator at a federal teaching hospital, speaking anonymously in March 2026.
The time spent negotiating consumes the remaining window for intervention.


The Hollow Core of Health Insurance
The National Health Insurance Authority (NHIA) is the official alternative. Its coverage tells a different story. As of the latest 2023 data, the NHIA covers approximately 16 million Nigerians. That is about 7% of the population.
The vast majority, including the informal sector, have no safety net. Wait, it gets more complex. For the few with insurance, emergencies are fraught with limits. Many plans impose co-payments. They have exclusion lists and caps. A comprehensive plan is N500,000 annual limit can be exhausted by one night in intensive care.
Doctors Without Tools
Assume a patient surmounts the financial hurdle. They then face a depleted system. The doctor-to-patient ratio is estimated at 1 doctor to over 5,000 patients. The World Health Organization recommends 1:600.
The shortage is compounded by a continuous brain drain. The Nigerian Medical Association stated that over 4,000 doctors left the country in 2023 alone, as Vanguard reported in 2024. Emergency rooms are staffed by exhausted professionals.
Basic diagnostics are a luxury. A 2022 assessment of secondary healthcare facilities across 20 states found that 65% lacked functional CT scanners. 80% had broken or obsolete ultrasound machines. Doctors make life-altering decisions based on intuition, not confirmed imaging.
The Budget Tells Its Own Story
The foundation of this crisis is budgetary. Based on the 2026 budget, the allocation to health is N1.33 trillion. The total budget is N49.74 trillion. It falls persistently below the 15% commitment made in the 2001 Abuja Declaration.
Per capita, the federal health budget translates to roughly N6,000 per Nigerian per year. Much is consumed by salaries. Little is left for infrastructure and emergency systems. In 2025, only about 65% of the capital health budget was disbursed for equipment. The funds often never arrive.
Funding for primary healthcare centers, the first line of defense, is particularly anemic. They lack ambulances, personnel, and drugs to stabilize emergencies.
“We have a pyramid that is inverted. We spend on tertiary care in cities, but the base of the pyramid, the primary centers that should prevent emergencies, is crumbling.” Dr. Muyi Aina, Executive Director of the National Primary Health Care Development Agency, in February 2026.
A Map of Survival Odds
Geography dictates destiny. Survival rates vary wildly between states. The National Bureau of Statistics indicated in 2025 that trauma mortality within 24 hours of hospital admission was three times higher in the North-East compared to the South-West.
This links directly to the concentration of specialist centers, paved roads, and networks. An accident on a remote road in Zamfara presents different odds than the same accident on the Lagos-Ibadan expressway.
The urban-rural divide is a chasm. In cities, private hospitals offer an escape route for those with means. They have modern equipment and specialists. Their fees place them beyond most citizens. They exist as a parallel system.

The Social Fabric as a Net
In the absence of a state safety net, Nigerians rely on social and religious networks. The first response is often a broadcast on WhatsApp groups, church assemblies, or mosque congregations. These networks raise funds, provide transport, offer moral support.
This community action is both resilience and an indictment of systemic failure. It transforms healthcare from a right into a charity. The speed and size of one’s social capital become critical.
Faith plays a visible role. Prayers are offered at accident scenes. This reliance on divine intervention is a logical response to a system that has proven unreliable. When science and the state are absent, people look heavenward.
One Practical Shift
A single, actionable change involves the protocol at public hospital gates. The federal and state ministries of health can mandate a “stabilize first, bill later” policy for genuine emergencies. This is enshrined in the National Health Act of 2014, which technically criminalizes refusal of emergency treatment.
Implementation demands a backup financing mechanism, like an emergency care fund. It could be seeded from a tiny percentage of the health budget. This shifts the priority from accounting to medicine in the first critical hour.
This change would not fix the ambulance shortage or the CT scanner. It would remove the most immediate and cruel barrier between a dying patient and a doctor. It replaces the finance officer with a medic at the point of entry.
The Arithmetic of Luck
Surviving a medical emergency here is a complex equation. Variables include proximity to a functional facility, liquidity of funds, competence of staff, functionality of equipment. The constant is chance.
The system, as structured, is a filter that sorts citizens by wealth and location. Those who survive often do so because a random set of circumstances aligned. A relative was nearby with cash. A doctor who trained abroad was on duty. A critical machine was working that day.
This reliance on serendipity is the opposite of a healthcare system. A system implies predictability and guaranteed access. What exists is a patchwork of contingencies.
The conversation about divine intervention arises because the human systems have left a vacuum. When the state is absent in the critical hour, people fill the void with faith, community, and hope against the arithmetic of probability.
The data shows a trajectory of stagnation. The budget percentages low. The doctor exodus continues. Infrastructure decays. Each emergency becomes a fresh test of individual fortune, a stark reminder that in the most vulnerable moment, one’s life depends on a roll of dice.
Rising Star’s Death Sparks Outrage: Can Nigerians Survive Medical Emergencies? , Nigerian Tribune. (Digital Illustration: GoBeyondLocal)
HealthCare
Local Herbal Drink Side Effects and Popular Brands in Nigeria
Are local herbal drink brands safe? We discuss side effects, market challenges, and Nigeria’s urgent need for regulation by 2026.


Millions of Nigerians consume local herbal drink products daily, with little knowledge of their contents or potential side effects.
The Thing About That Bottle
Published: 03 April, 2026
You see them in traffic, in markets, and in corner shops. Brightly colored bottles with labels promising relief from pile, stomach pain, or malaria. These local herbal drink concoctions, often called Agbo, form a multi-billion naira informal industry. According to a 2025 report in Premium Times, the National Agency for Food and Drug Administration and Control has registered over 13,000 herbal medicines. The actual number of unregistered products circulating in the market remains a mystery.
Here is the thing. Many consumers believe these products are inherently safe because they are natural. This belief drives a massive, mostly unregulated market. A report from the World Health Organization in 2025 noted that up to 80% of the population in some African countries uses traditional medicine for primary healthcare. In the context of Nigeria, this translates to a heavy reliance on these bottled mixtures.
What Is Actually In The Drink
Let us break it down. A typical local herbal drink contains a blend of roots, barks, leaves, and seeds. Common ingredients include ginger, garlic, lemon grass, and bitter kola. The problem starts with preparation. There is no standard dose. One maker uses a handful of leaves, another uses two.
Scientific analysis reveals more. A 2025 study published in the Journal of Ethnopharmacology tested 45 popular Agbo samples from Lagos markets. The study reported that 34% of the samples contained undeclared pharmaceutical drugs, including painkillers and steroids. Another 23% had heavy metal contamination above safe limits. You are drinking more than herbs.
Brands You Know And The Risks They Carry
So here we are. You recognize the names. Brands like Agbo Jedi Jedi for pile, Opa Eyin for eye issues, and Agbo Ibà for fever dominate the landscape. These products have become household names through word-of-mouth and aggressive street marketing. Their efficacy is an article of faith for many.
Yet, clinical evidence is scarce. The side effects range from mild to severe. Common complaints include acute stomach upset, diarrhea, and dizziness. More serious cases involve liver damage and kidney injury. According to a 2026 report in The Guardian Nigeria, a teaching hospital in Ibadan documented a 15% rise in cases of liver toxicity linked to herbal medicine from 2024 to 2025. The patients cited popular brand names.
The Liver And Kidney Question
The liver processes everything you consume. Some herbs contain compounds that are toxic to liver cells with prolonged use. The kidney filters waste from the blood. Contaminants like heavy metals accumulate and cause irreversible damage. These organs work silently, so damage often goes unnoticed until it becomes critical.
Professor Abdulsalami Nasidi, a public health consultant, highlighted this point.
“The absence of immediate adverse effects creates a false sense of security. Chronic toxicity from repeated consumption of unstandardized herbal mixtures presents a silent public health challenge.”
— Professor Abdulsalami Nasidi, public health consultant, in The Nation (March 2026)


The Regulatory Gap Is A Canyon
NAFDAC has a mandate to regulate all consumables. The agency operates a registration process for herbal medicines. Manufacturers submit details about their ingredients and production process. Upon approval, they receive a registration number for their label.
Reality check. The informal market is vast. Many producers operate without any registration. Even for registered products, post-market surveillance is weak. In 2026, NAFDAC has intensified its “Yellow Label” initiative for verified traditional medicines — a specific identifier that helps consumers distinguish certified products from unregulated ones. However, according to a 2025 report in BusinessDay, a NAFDAC director conceded at a stakeholders meeting that logistical challenges continue to hinder comprehensive market monitoring. The system relies heavily on complaints before investigation.
Why Enforcement Stumbles
Think about the supply chain. Production happens in small, scattered workshops. Distribution uses thousands of informal vendors. This decentralized model makes tracking difficult. Enforcement officers focus more on large-scale, packaged food and drug fraud. The woman selling single bottles in a basket often escapes scrutiny.
Cultural acceptance also shields the industry. Many citizens view regulation as government interference in traditional practice. This sentiment creates a social barrier for effective control. The seller is a neighbor providing a trusted service, not a criminal.
Stories From The Hospital Ward
Medical doctors have stories. Dr. Chioma Mbonu, a gastroenterologist in Abuja, sees the consequences. She recounted a case from late 2025. A man in his forties came with severe jaundice and abdominal pain. He had consumed a popular local herbal drink for stomach ulcers for three months. Tests confirmed drug-induced hepatitis linked to the herbal mixture.
“Patients often do not disclose herbal use during consultation. They consider it irrelevant or fear judgment. This information gap delays correct diagnosis and appropriate treatment.”
— Dr. Chioma Mbonu, gastroenterologist, interview with Vanguard (February 2026)
These cases are underreported. Patients seek care at traditional healers first or use another herbal mix to counter the side effects of the first. By the time they reach a conventional hospital, the condition is advanced.
The Economic Pull Is Strong
Forget the health talk for a minute. This is about livelihood. Selling Agbo provides income for countless families. The barriers to entry are low. You need some knowledge of herbs, bottles, and a small capital. This economic reality guarantees the market continues to thrive.
The appeal is also financial for the consumer. A bottle of Agbo costs a fraction of a doctor consultation fee or prescribed antibiotics. In an economy with high out-of-pocket health expenditure, this price difference is decisive. People manage their health with the resources they have.


A Path Forward Exists
This situation requires a pragmatic solution. A wholesale ban would fail and push the trade further underground. The goal should be harm reduction and quality improvement. Integration of traditional medicine into the formal health system offers a viable model.
NAFDAC launched the Herbal Medicine Product Registration Acceleration Initiative in 2024. The program aims to bring more producers into the regulatory fold by simplifying paperwork. According to the NAFDAC Official Bulletin in 2026, the agency reported a 20% increase in applications from herbal practitioners as of March of that year. This is a positive step, but scale is necessary.
What You Can Do Today
Your health is your responsibility. You make choices every day. If you choose to use a local herbal drink, apply basic consumer wisdom:
- Look for the NAFDAC registration number on the label. A missing number is a red flag.
- Look for the “Yellow Label” — NAFDAC’s 2026 initiative for verified traditional medicines.
- Purchase from reputable vendors, not random hawkers.
- Listen to your body. Discontinue use if you experience unusual symptoms like prolonged nausea, yellow eyes, or reduced urination.
- Inform your doctor about every substance you ingest, including herbs. This disclosure helps them protect you.
The Final Word On Herbal Drinks
Traditional medicine has a place in the culture of Nigeria. It offers accessibility and cultural resonance. The challenge lies in ensuring its safety for the population. The current system, with its gaps, exposes millions to preventable risk.
Progress depends on collaboration. Regulators, practitioners, and consumers each have a role. Producers must embrace standardization. Authorities must enhance monitoring. Citizens must demand quality. The story of local herbal drink in Nigeria is still being written. The next chapter needs more science and less guesswork.
Publication Date: April 02, 2026. This article is based on available reports and expert statements as of March 2026. Market dynamics for unregulated products are fluid and data on total consumption remains estimated.
Disclaimer: This article is for informational purposes and does not constitute medical advice. Always consult a licensed healthcare professional before starting any herbal treatment.
Understanding Herbal Medicine Safety in Nigeria – Relevant coverage on this topic.
HealthCare
Dark Skin Skincare for Nigerian Weather and Glow
Struggling with dark skin skincare in Nigeria’s heat? Get your 2026 glow with proven tips for hydration and sun protection.


The sun in Lagos feels different from the sun in Abuja. Humidity in Port Harcourt makes your skin behave in ways you never expected. A dark skin skincare routine for the heat of Nigeria requires a specific plan. The goal is a healthy glow, not just a temporary shine.
Your Skin Is Talking, Listen to the Weather
Published: 03 April, 2026
High temperatures and humidity define the climate of Nigeria. According to NOAA Climate.gov’s 2025 data, average temperatures in southern regions remain above 30°C for much of the year. This heat accelerates transepidermal water loss.
Humidity levels often exceed 80%. This moisture in the air can create a deceptive feeling of hydration. The skin may produce excess sebum as a confused response. A routine must balance hydration with managing this oil production.
Dust and pollution in urban centers like Lagos and Kano add another layer. These particles settle on the skin. They mix with sweat and sebum. This mixture can clog pores and lead to breakouts.
Forget Everything You Think You Know About Sunscreen
Many people with dark skin believe they have natural sun protection. Melanin provides a Sun Protection Factor of about SPF 13. According to a 2025 article in the Journal of the American Academy of Dermatology, this is insufficient for the intensity of the sun in Nigeria.
Ultraviolet radiation remains the primary external cause of premature aging. It also triggers hyperpigmentation. A broad-spectrum sunscreen with at least SPF 30 is non-negotiable. Reapplication every two hours is essential with sweating.
2026 Expert Tip: For dark skin, traditional mineral sunscreens (zinc oxide or titanium dioxide) often leave a “white cast” or purple hue. Look for “Invisible Finish” or “Tinted Mineral Sunscreens”. Modern chemical filters like Tinosorb are also excellent options that blend seamlessly into melanin-rich skin.
“The idea that darker skin tones do not need sunscreen is a dangerous myth. We see the consequences in our clinics: persistent dark spots and textural changes directly linked to sun exposure.”
Dr. Ifeoma Nwankwo, Consultant Dermatologist, Lagos University Teaching Hospital, in an interview with Vanguard (March 2026)
Hydration Is a Full-Time Job, Not a Morning Task
The heat pulls water from your skin throughout the day. A light, water-based moisturizer is your best friend. Ingredients like hyaluronic acid and glycerin (a humectant) attract water molecules. They help bind moisture to the skin.
2026 Climate Tip: In high humidity (like Port Harcourt), humectants like glycerin actually pull moisture from the air into your skin, making them more effective than in dry northern climates. This is a game-changer for understanding how your skin behaves.
Heavy creams and butters can trap too much heat. They may feel suffocating in humidity. A gel-cream hybrid texture often works well. It provides hydration without a greasy film.
Internal hydration matters as much as topical products. Drinking adequate water supports skin elasticity. It helps flush toxins. Carry a water bottle. Make it a habit.


The Real Enemy Has a Name: Post-Inflammatory Hyperpigmentation
This is the technical term for the dark marks left after a pimple heals. Skin with more melanin has a higher propensity for this reaction. A single spot can leave a mark that lasts for months.
The first line of defense is to avoid picking or squeezing blemishes. This trauma worsens inflammation. It signals the melanocytes to produce more pigment. Keep your hands away from your face.
Incorporating gentle chemical exfoliants helps. Alpha hydroxy acids like glycolic acid or lactic acid encourage cell turnover. They fade existing marks. They prevent new ones from forming so deeply.
“In our humid environment, acne is common. The lasting issue for patients with darker skin is rarely the acne itself, but the hyperpigmentation it leaves behind. Prevention is infinitely easier than treatment.”
Dr. Chidi Nwosu, Dermatologist at The Skin Clinic, Abuja, speaking to Punch (February 2026)
Cleansing Is the Foundation, Do It Right
You need to remove sweat, oil, and pollution without stripping your skin. A gentle, sulfate-free cleanser is ideal. Use it twice daily, in the morning and evening.
In the evening, consider a double cleanse if you wear sunscreen or makeup. Start with a micellar water or a light cleansing oil. Follow with your regular water-based cleanser. This ensures a thorough clean.
Water temperature matters. Use lukewarm water. Hot water can disrupt the skin barrier. It can increase redness and sensitivity over time.
Ingredients That Work With Your Skin, Not Against It
Niacinamide is a superstar ingredient for dark skin. It regulates oil production. It strengthens the skin barrier. It helps reduce the appearance of dark spots. Look for concentrations between 5% and 10%.
Vitamin C is a potent antioxidant. It protects against environmental damage. It also inhibits the enzyme responsible for melanin production. This makes it excellent for brightening and evening skin tone.
Retinoids, like retinol, promote collagen production and cell turnover. They are effective for treating acne and fading marks. Start with a low concentration. Use it only at night. Always follow with sunscreen in the morning.
What a Simple Daily Plan Looks Like
Morning: Start with a gentle cleanse. Apply a vitamin C serum on damp skin. Follow with a light moisturizer containing niacinamide. Finish with a generous amount of broad-spectrum sunscreen (tinted or invisible finish).
Evening: Begin with a double cleanse if needed. Use a gentle exfoliating toner with AHAs, perhaps three times a week. On other nights, apply a retinol serum or a treatment for dark spots. Lock everything in with a moisturizer.
Consistency brings results. A complicated routine is difficult to maintain. Simplicity wins in the long term. Choose products that serve multiple purposes.
When to See a Professional
Persistent acne or severe hyperpigmentation may need prescription strength. A dermatologist can provide treatments like hydroquinone, tretinoin, or chemical peels. These are regulated and used under supervision.
Do-it-yourself treatments with harsh chemicals are risky. They can cause burns or permanent discoloration. The market for skin lightening creams is large and poorly regulated.
NAFDAC 2026 Warning: In early 2026, NAFDAC issued a specific alert regarding Mercury and Hydroquinone in “fast-action” brightening creams sold in open markets like Balogun (Lagos) or Onitsha. These ingredients are dangerous and banned. Always check for NAFDAC registration numbers.
Investing in a consultation with a board-certified dermatologist saves money and prevents damage. They provide a diagnosis and a safe, effective plan.
Your Skin on a Budget
Effective skincare does not require the most expensive products. Local pharmacies and reputable online stores carry good options. The key is reading ingredient lists, not just brand names.
Sunscreen is the most important purchase. An affordable, effective sunscreen used daily offers more benefit than an expensive serum used sporadically. Prioritize your spending.
Some natural ingredients have merit. Aloe vera gel is soothing. Green tea has antioxidant properties. Use them as supplements to a core routine, not as replacements for proven actives.
Make This Your New Normal
Start by auditing your current products. Check their expiry dates. See if they are suited for humid weather. Introduce one new product at a time. Wait two weeks before adding another.
This approach helps you identify what works. It also helps you pinpoint any product that causes a reaction. Patience is part of the process. Your skin will adjust.
The glow comes from health. Hydrated, protected, and well-cared-for skin has a natural luminosity. It reflects light beautifully. That is the goal.
Skincare is a form of self-care. In the hustle of Nigerian life, taking those few minutes morning and evening is a quiet act of maintenance. The heat is constant. Your routine can be a constant too. Your skin will thank you for the consistency.
THE BEST BODY LOTIONS FOR DARK/CARAMEL SKIN TONE | Effective and Affordable #glowcream – Relevant coverage on this topic.
HealthCare
Nigeria Hypertension Risk: Urban Diets and Exercise Extend Lives
Struggling with high blood pressure in Lagos or Abuja? New 2026 data proves better urban diets and exercise directly lower Nigeria hypertension risk.


Nigeria Hypertension Risk: Urban Diets and Exercise Extend Lives
Published: 25 March, 2026
Thirty-five per cent of adults. That was the scale of the crisis in Nigeria just last year. Hypertension is the major killer. But first-quarter data for 2026 suggests a shift is happening in the cities. Deliberate changes in kitchens and on sidewalks are starting to bend a deadly curve. They are adding years to urban lives.
The trouble is, the baseline was a disaster. Urban life built a perfect trap: greasy fast food and desk-bound roles, a breeding ground for strokes. The Federal Ministry of Health reported on March 12, 2026, that an estimated 35 per cent to 40 per cent of adults in 2025 had high blood pressure. We built a health system for malaria and childbirth. For decades, we left this chronic crisis to fester.
The Heavy Truth About Urban Pressure
So what changed? Look first to the kitchen. A quiet, pragmatic revolution is underway. It is less about formal diets, more about substitution. Health concerns and cost are the main drivers. A general trend of Nigerians reducing consumption of processed foods is now evident.
People are returning to swallows like amala and eba, but with more vegetable soups and less oily stews, said Dr. Chioma Nwakanma, a public health nutritionist in Lagos. The awareness is sinking in.
The data from our community screenings in Surulere and Ikeja shows a 15% lower prevalence of stage 2 hypertension among adults who report high vegetable consumption, compared to those who do not. The message about reducing palm oil and salt is getting through, one kitchen at a time, Dr. Chioma Nwakanma, interview with The Guardian, February 2026.
Supermarket aisles confirm it. Sales of low-sodium stock cubes and salt substitutes have seen significant increase. This change is driven by urbanites who have received a hypertension diagnosis. Reactive at first. Then it becomes a habit.

A professional monitors their health while incorporating fresh fruit into their daily routine. (Digital Illustration: GoBeyondLocal)
The Streets Are for Walking Again
Now look outside. Exercise is ceasing to be a foreign concept. The most significant change is the normalization of walking. In Abuja, Millennium Park and the green areas in Maitama are filled with walkers at dawn. In Lagos, the state government cleanup of sidewalks in Ikoyi and Victoria Island has made walking less hazardous.
Organized running clubs have exploded. The Access Bank Lagos City Marathon took place on Saturday, February 14, 2026. Kenyan runner Ezra Kipchumba Kering won the 42km race with a time of 2:11:55. From this flagship event to weekly park runs in Port Harcourt, running is now social. Corporate wellness programs add another layer. Companies are investing in employee health initiatives.
The Numbers Start to Tell a New Story
This brings us to the impact. Preliminary data is showing results. An interim by the Nigeria Centre for Disease Control in 2026 points to a stabilization, even a slight decline, in hypertension rates among urban adults under 50. The national burden remains critically high, but the urban curve is flattening.
Contrast this with the World Bank data for 2023, which put average life expectancy at approximately 54.5 years. The lifestyle modifications in cities are directly preventing cardiovascular events.
Our models suggest the lifestyle modifications in cities, less dietary salt, more aerobic activity, are directly preventing cardiovascular events. For every 10% increase in reported moderate exercise in a population, we see a correlating 2-3% drop in hypertension-related hospital admissions. The link is evident, Prof. Ibrahim Danjuma, African Journal of Medicine, December 2025.
Why This Might Not Be Enough
But there is a catch. This progress is fragile and concentrated. It lives among the educated, middle-class urban population. The urban poor, in crowded estates with limited access to fresh food and safe spaces, continue to be extremely vulnerable. For them, the risk is unchanged or worsening.
Government policy has been slow. A bill to amend the excise duty framework for Sugar-Sweetened Beverages is currently before the Senate. Sponsored by Senator Ipalibo Harry Banigo, it seeks to increase the Basic Health Care Provision Fund from 1% to 2% of consolidated revenue. Advocates are pushing for a 50% retail levy. The current N10 tax has become negligible due to inflation.


A composition health tools, a blood pressure monitor, fresh fruit, water, and fitness tracking, representing proactive lifestyle management. (Digital Illustration: GoBeyondLocal)
The Policy That Could Change the Game
One policy could change the game. It is simple: mandatory hypertension screening at every primary health contact. Go to a clinic for malaria, get your blood pressure checked. Bring a child for immunization, get your blood pressure checked. This opportunistic screening model is cost-practical. It creates massive data.
Wait, it gets more complex. The reality of primary healthcare centers tells a revealing story. According to NCDC-backed research from March 2026, while 98% of urban Primary Healthcare Centers have working blood pressure apparatus, only 24% have the clinical guidelines to treat the patients they diagnose. This readiness gap is the missing link.
The Lagos State Government piloted opportunistic screening in 2024. The 2025 evaluation showed a 300% increase in new hypertension case detection in one year. It linked 65% of those newly diagnosed to care. Scaling this nationally would require training and simple equipment. The investment is modest compared to the cost of treating strokes.
Your Next Move This Week
For you, the action is personal and immediate. The most practical step is to know your own numbers. A blood pressure check takes two minutes. It is often free at pharmacy outlets in major cities.
Make that check this week. If the reading is high, that information is power. It starts a conversation. It motivates one less stock cube in the pot, one more serving of vegetables. It justifies a 30-minute walk. The entire national change is built on millions of decisions like that one. The data proves those decisions are now adding years to lives in the cities. The task is to make that truth spread beyond the city limits.
Kenya’s Ezra Kering Wins 2026 Lagos Marathon , Channels Television. (Digital Illustration: GoBeyondLocal)



 Edutech Portal2 months ago
Edutech Portal2 months agoInternet Sovereignty: Why Some Countries Want Their Own Separate Internet



 Edutech Portal2 months ago
Edutech Portal2 months agoThe Story Of The Nigerian Who Helped Build Global Internet Systems



 Edutech Portal2 months ago
Edutech Portal2 months agoNigerian Hackers: The Global Fraud Story and Its Fallout



 Edutech Portal2 months ago
Edutech Portal2 months agoForgotten Satellites Defy Silence, Beaming Signals for Decades



 Edutech Portal2 months ago
Edutech Portal2 months agoYour Digital Store in Nigeria and the Reality of Domain Expiration



 Edutech Portal2 months ago
Edutech Portal2 months agoThe Phone Stay So Quiet: An Investigation into Nigeria’s Silent Customer Lines



 Edutech Portal2 months ago
Edutech Portal2 months agoThe Business That Died: A Nigerian Case Study in Refusal to Adapt



 Edutech Portal2 months ago
Edutech Portal2 months agoHiding Your Business From People With Money
























